Dr Jeejesh Kumar [ 4 Jan 2011]
This 32 year old lady, mother of 2, who has been hopping on one leg for the
last 10 years or so. now comes with pain in the proximal femur (at prominence of the k nail).
she wishes to get rid of the pain and improvement of the deformity only if
we are sure that that she will do well.
she was diagnosed as fibrous dysplasia at age of 10 yrs, has had multiple
surgeries for correction of the deformities, last one being the k nail 10 years ago.
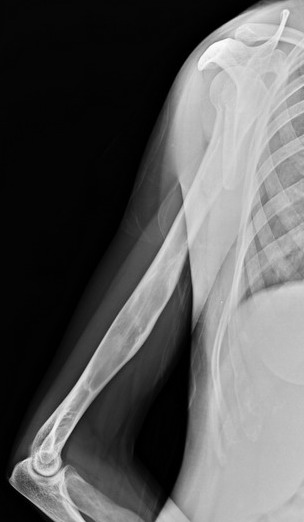
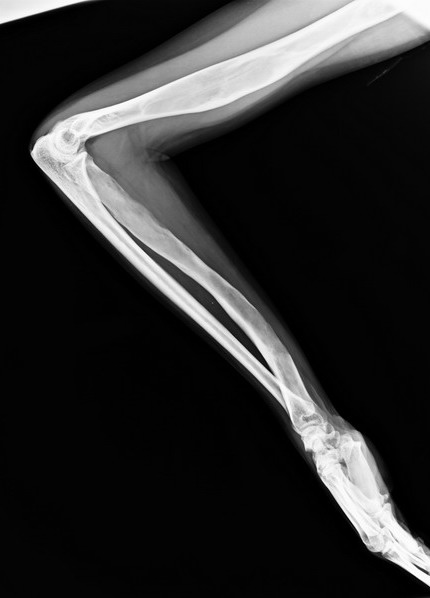
she has similar lesions in the radius-ulna and humerus on the same side but mild deformity, no functional deficit.
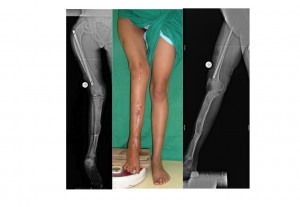
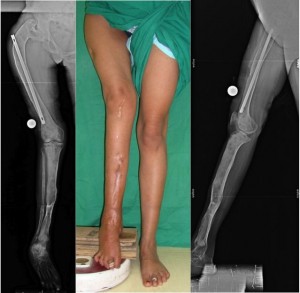
full length xrays and clinical pictures are attached.
blood investigations wnl.
your suggestions invited for modalities of treatment.
1. removal of nail only
2. correction of deformities - femur only? femur and equinus together? femur and equinus staged?
3. any expected problems in healing? any specific medications?
Reply to author
Dr Bijayendra Singh
It would be interesting to see what her immediate correction was?
If this was done only 10 yrs ago, then looking at her radiographs, perhaps
not likely, or maybe it was done before maturity.
At present we need to know - shortening? looking at your pictures I would guess around 3 inches. What are her hip & knee movements? Where is the pain?
What’s her gait like? I think if she only wants to get rid of the pain at the insertion, then perhaps just removal might do the trick.
Do you have clinical & radiographs of the other affected limb?
Bijayendra Singh,
Medway NHS Foundation Trust, UK
www.kosis.co.uk
Dr Jeejesh Kumar
Dear Bijayendra sir, Her pain is in the proximal femur at the prominence of the K nail that I have already mentioned. Her shortening is about 10 cm. Knee ROM is 0 to 120 degree There is no abduction at the hip and adduction is shown in the picture and it is more than 45 degree. Internal rotation is full and there is no external rotation at the hip. She walks with crutch without putting weight on the affected leg like hopping
Dr.T.K.Jeejeshkumar DNB
Clinical fellow in Ilizarov and limb reconstruction
CLLR.Mumbai
-Bharat
Sir,
Thank you for sharing interesting cases on this group. If I may seek Some clarifications-
1) Was there any other problem with gait prior to this pain? Was 'hopping' attributed to a short limb gait (+/- trendelenberg lurch) alone on examination?
2) From the X-ray, ankle doesn't seem to have any ROM-is that correct?
3) Was there any symptom or consultation to suggest disease activity over the last ten years?
4) Does the deformity interfere with any function, other than walking?
Regards,
Bharat Sharma
D.ORTH (Jipmer) DNB MPEB (IIMB)
-DOMINIC PUTHOOR
Hope Ilizarov experts will have something to tell about its management. Expecting reply from Mangal, Vasudevan, or Cherian.
Dominic
Dr Jeejesh Kumar
Dear Dr.Bharat,
1. no other problem with gait. she hopped because that was the best way that she could get around (as per her statement). trendelenberg could not be tested as she has no abduction even passively
2. the ankle is fused in equinus
3. no disease activity. she was 'carrying on' and claims that she did not see any hope of getting better. went to a local orthopod for the pain that developed at the k nail insertion site, who in turn directed her to us.
4. she has borne two children, and is a housewife, who apparently carries out her routine activities/duties
.
Dear Dr.Bijayndra,
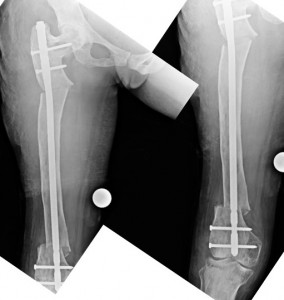
I am uploading her x-rays of upper limb
Dr.T.K.Jeejeshkumar DNB
Clinical fellow in Ilizarov and limb reconstruction
CLLR.Mumbai
Dr Ramanathan.ortho ipoh.malaysia
Jeejesh
This is mcune- Albright syndrome.pl also look for skin pigments, renal condi etc. Residronate has been tried, no significant success. Replacing some fibrous areas with autograft assisted by b.m.p. (protein) and of course stabilizing the bone in the best way in your hands helps.
Cheers
Dr Vasudevan
Dear Jijesh,
Jijesh is Mangal's fellow.
I am for removal of the implants and custom made ILN from knee up with locking screws into the head and multiple osteotomies where ever it stucks. No Ilizarov and no limb lengthening now. ( U have to design a nail for that!!!!!!!!!!!!!!!! 😉
PFN like nail is better but it may be difficult to get an entry from trochanter.
Do not struggle too much.
Now I am also in a similar situation similar patient had come with sub troch # and with h/o previous infection. And I am stuck. I think I will do an Ilizarov on him. ;(
Good luck
Dr. Vasudevan. PN,
Consultant Orthopedic Surgeon,
RV Institute of Research in Ilizarov Technology,
West Fort Road, Palakkad, Kerala.
Dr Jeejesh Kumar
Dear Dr.Ramanathan
Here the patient has no classic triad (Cafe-au-lait spot ,autoimmune endocrine dysfunction,polyostotic fibrous dysplasia) of the syndrome Polyostotic fibrous dysplasia(Albright's disease) is a form of fibrous dysplasia affecting more than one bone.
McCune-Albright syndrome include Polyostotic fibrous dysplasia as a part of its presentation.
Dr.T.K.Jeejeshkumar DNB
Clinical fellow in Ilizarov and limb reconstruction
CLLR.Mumbai
Dr Ramanathan.ortho ipoh.malaysia
Dr Jeejesh
U mentioned in Ur first mail that the pt has it also in the radius ulna n humerus on the same side
Bijayendra Singh
I think given her problems, perhaps correcting the femur with osteotomies & ILN would be useful. The equinus may be beneficial as she has shortening. As for the upper limb unless any specific deformity, leave it well alone.
Bijayendra Singh,
Medway NHS Foundation Trust, UK
www.kosis.co.uk
DOMINIC PUTHOOR
Dear Dr. Vasudevan,
Why '*No Ilizarov and no limb lengthening now *'. Is it because of pathology of the lesion? I personally feel fibrous dysplasia being a non neoplastic condition will regenerate healthy bone on distraction. But have no personal experience.
DOMINIC
Jay Sampath
I did a very similar case in a 13 year old lad. The problem with fibrous dysplasia is that the enlarged medullary canal is of a variable density along the entire length of the bone. Guide wires do not necessarily follow a straight path due to presence of these dense islands and tend to get stuck. Blood loss is significant. Original plan was to do a subtroch valgus osteotomy and recon locking in addition to correcting the diaphyseal deformity but due to my lack of familiarity with temperamental Indian instrumentation and implants, we just ended up straightening the leg and bolting it all together. Percutaneous osteotomies and external fixation might be safer after removal of the current IM nail. Our case should be coming for his 2 month follow-up shortly.
Jay Sampath
Dr Murali Poduval
Dear Jijesh
Interesting case. The nail of course has to come out but you can’t stop there. There would be a cortical defect, and however small, there is a risk of fracture through the defect of nail removal, as the bone itself is abnormal. You would have to correct the femoral deformities and in the process would gain some length, while abducting the femur, I have, in the few cases I did, resected some bone to ease apposition. I did try nailing once but landed up in trouble, the guide wire got stuck, I had problems accessing the entry point even through the retrograde (through fracture site) method. I ended up using a 95 degree plate, rather long. The patients I did were young, one I had posted results some years ago I think. Still, even at this age, I wouldn’t anticipate any problems with healing. I dare say that IM nailing with the current expertise available at your center would be the ideal choice for fixation. I would not prefer flexible nails but would prefer a locked IM nail. The equinus and lengthening of the limb , at least in my opinion , be tackled as a second stage procedure. This time a ring would be the only choice for me.
Do let us know how you have planned and executed this difficult deformity
Thanks for putting up the unusual and stimulating case for discussion.
Regards
Dr Murali Poduval
Senior Associate Professor
Faculty of Medicine, Department of Orthopedics
AIMST University Kedah Darul Alam Malaysia
Dr Vasudevan
Dear Dominic.
In this patient, she had almost accepted her disability of shortening etc.
Her presenting problem is only pain. After implant removal there is a high risk of stress #. So it is better to realign the limb. As the bone is weak I doubt about the holding power of the ex fix on to it for an extensive limb lengthening, u have to keep it for a longer period. And more over there are reports on fibrous dysplasia developing sarcomatous changes after distraction ( read many years back). In general I prefer titanium nail in fibrous dysplasia than any fixator and if there is no option then I will definitely do it.
Dr. Vasudevan. PN,
Consultant Orthopedic Surgeon,
RV Institute of Research in Ilizarov Technology,
West Fort Road, Palakkad, Kerala.
Dr Mangal Parihar
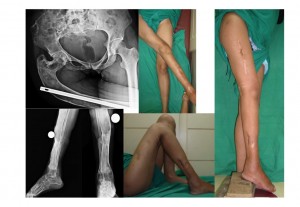
here is what was done for the patient. this was achieved with a wedge excision at the proximal osteotomy, and percut osteotomy at the distal. nothing specific (curettage etc) was done for the "fibrous dysplasia"
slide 2a - Preop plan with simulation of correction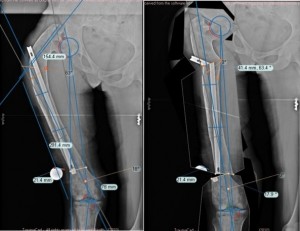
slide4a - one intraop picture to show the extent of the bowing in the proximal part, and post op clinical (10 days post op)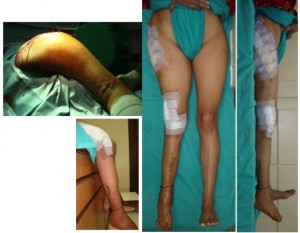
she went home partial weight bearing with a walker.
at a second stage we plan to correct the tibial deformity and equinus of the foot.
mangal Parihar
DOMINIC PUTHOOR
Thank you Dr Mangal. Now I understand that deformity correction does not always means Ilizarov.
Domiinc
Jay Sampath
Hi Mangal
Lots of lines on the long leg x-rays and virtual osteotomies. Is that TramaCAD? Will send the paper in due course, it's hidden somewhere in the hard drive.
Jay
Dr Mangal Parihar
yes. TramaCAD.
mangal
Vijay chichani
dear dr mangal, did u need adductor tenotomy/was there free abduction possible at the end thanks
Dr.Vijay M Chichani
D ortho M.S.ortho (Mumbai)
Nanded.
Badri Narayan
Have you tried the newer version of TramaCAD for deformity analysis - it is quite stunning in its simplicity. It finds CORAs, and even multiple CORAs if you need it to, and it even does virtual simulations of corrections - one step faster than the 'define fragments' method.
Badri Narayan Orthopaedic Surgeon Feb 9, 10:50 am
Dr Mangal Parihar
We did an adductor tenotomy after turning the patient into supine.
Abduction was possible.
Dr Mangal Parihar
Dr Mangal Parihar
Yes. It’s now a part of orthoweb.com , That's what this planning was done with. "Auto deformity"
Mangal




 India-Orth
India-Orth