Introduction
Spinal cord injury without radiographic abnormalities (SCIWORA) has been classically described in pediatric cervical spine injuries. This acronym was coined by Pang and Wilberger in 1982 to denote presence of clinical findings (neurological deficit) in the setting of normal X Rays and Computerized Tomographic (CT) Scan. The advent of Magnetic Resonance Imaging (MRI) has made it possible to accurately characterize the underlying spinal cord injury even when radiographs and CT scan are normal.
SCIWORA should now be more correctly renamed as "spinal cord injury without neuroimaging abnormality" and recognize that its prognosis is actually better than patients with spinal cord injury and radiologic evidence of traumatic injury.
Definition
In view of these advances, Pang reviewed his work in 2004 and advocated that only cases with neural injuries seen on MRI or those with normal MRI findings should be counted as SCIWORA and purely extra neural compressive lesions should be excluded from the definition of SCIWORA.
Prevalence
- occurs most often in pediatric population; range from birth to 16 yrs
- a true incidence is probably close to 20% of all pediatric spinal cord injuries
- accounts for up to 30% of severe cervical injuries in children 8 years of age and younger
- 10% in children 9-16 yrs
- children < 8yrs have worse prognosis.
- cervical, thoracic SCI common, lumbar rare.
Pathogenesis
In pediatric population:
SCIWORA was described by Pang and Wilberger in 1982 in the pediatric cervical spine. Inherent elasticity of the vertebral column due to ligamentous laxity, combined with the large head size predisposes the pediatric cervical spine to deforming forces. Pang described four mechanisms of SCIWORA viz. flexion, hyperextension, longitudinal distraction and ischemia.
In adult population:
The pathophysiology of adult SCIWORA is quite different from that of pediatric population. Most cases are due to hyperextension injury to the spine, which may be seen in rear end motor vehicle collisions or direct anterior craniofacial trauma. Another peculiar feature is preexisting cervical spondylosis, which predisposes to cord injury even with trivial trauma. Kasimatis et al have suggested that elderly patients with spondylosis have posterior vertebral spurs and ligamentum flavum bulging due to decreased vertebral body height. Hyperextension injury in such cases, even if trivial, can result in a central cord syndrome. adult SCIWORA comprises of a three patterns of neural injuries viz. hemorrhage, edema and contusion. Cord edema has the best prognosis and cord haemorrhage has the worst. Longitudinal signal extension and multiple extra neural injuries are associated with poorer outcomes. Purely extra neural compressive pathologies are best regarded as separate entities and should not be merged with SCIWORA.
Neurological presentation:
SCIWORA can have a wide spectrum of neurological dysfunction, ranging from mild, transient spinal cord concussive deficits to permanent, complete injuries of the spinal cord. The incidence and severity of injury are related to the patient’s age. Young children have a higher incidence of SCIWORA; this age group accounts for two-thirds of all reported cases. Adolescents sustain less severe, typically incomplete injuries. A delay in the onset of neurological deficits or a delayed neurological deterioration had been reported. Brief transient motor or sensory symptoms are often associated with the initial injury. An asymptomatic period usually intervenes. The delays in deficits can range from hours to 4 days after injury.
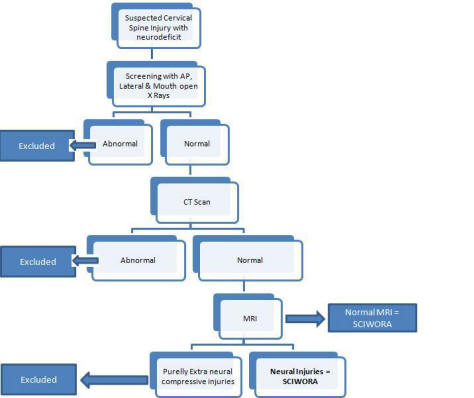
Algorithm to diagnose SCIWORA
Options:
- Plain spinal radiographs of the region of injury and CT scan with attention to the suspected level of neurological injury to exclude occult fractures are recommended.
- MR of the region of suspected neurological injury may provide useful diagnostic information.
- Plain radiographs of the entire spinal column may be considered.
- Neither spinal angiography nor myelography is recommended in the evaluation of patients with SCIWORA.
Diagnosis of exclusion:
- MRI may give a more anatomic diagnosis by showing hemorrhage or edema of the spinal cord;
- pseudosubluxation: anterior displacement may be up to 4 mm;
- SSEPs: Somatosensory Evoked Potentials, are electrophysiologic response of nervour system to sensory stimulation, used not diagnostically, but to test neurologic function, can relate any decrease or absence of impulse transmission through the spinal cord, obtained within 24 hrs of admission and compared in follow up analysis.
Differential diagnosis
- Traumatic compressive myelopathy (compression by fractured vertebrae, disc herniation etc)
- Acute disseminated encephalomyelitis
- Transverse myelitis
Treatment
Spine is immobilized for one to three weeks;
Standards: There is insufficient evidence to support treatment standards.
Guidelines: There is insufficient evidence to support treatment guidelines.
Options:
- External immobilization is recommended until spinal stability is confirmed flexion and extension radiographs.
- External immobilization of the spinal segment of injury (collar or a more rigid brace) for up to 12 weeks may be considered.
- Avoidance of "high-risk" activities for up to six months following SCIWORA may be considered.
- Hard collar immobilization for patients with cervical level SCIWORA for 12 weeks
- avoidance of activities that encourage flexion and extension of the neck for an additional 12 weeks has not been associated with recurrent injury.
- After the acute phase of injury, it is advisable to repeat the flexion/extension views of the spine to rule out ligamentous instability that may have been masked by paravertebral muscle spasm during the initial evaluation
- Once deficits have resolved range of motion is gradually increased.
- To avoid the risk of recurrent injury, activity should be strictly limited for at least 3 months.
- High dose steroids
- Methylprednisolone bolus of 30 mg/Kg iv within 8 hr s of injury, followed by infusion at 5.4 mg/Kg/hr for the next 23 hrs is beneficial in improving the outcome.
- When given over 48 hrs outcome at 6 wks and 6 months was better in a recent study.
- Role of stem cell transplant is emerging.
Nursing Management:
- spine stabilization,
- patient & parents counseling & explanation,
- regular neuro assessment;
- caution in turningpositioning,
- suctioning,
- prevention of complications like pressure sore, pulmonary side effect, contractures.
Conservative management of purely neural injuries yields good results, but the presence of coexistent extra neural injuries, especially disc prolapse and ligamentous instability requires surgical management.





 India-Orth
India-Orth